Cardiovascular & Respiratory system
- Created by: Charlotte170289
- Created on: 08-01-21 11:54
The main structures
Cardiovascular system:
- Heart
- Systemic blood vessels
Respiratory system:
- Upper and lower airways
- Lungs
- Pulmonary blood vessels
Cardiovascular & Respiratory system
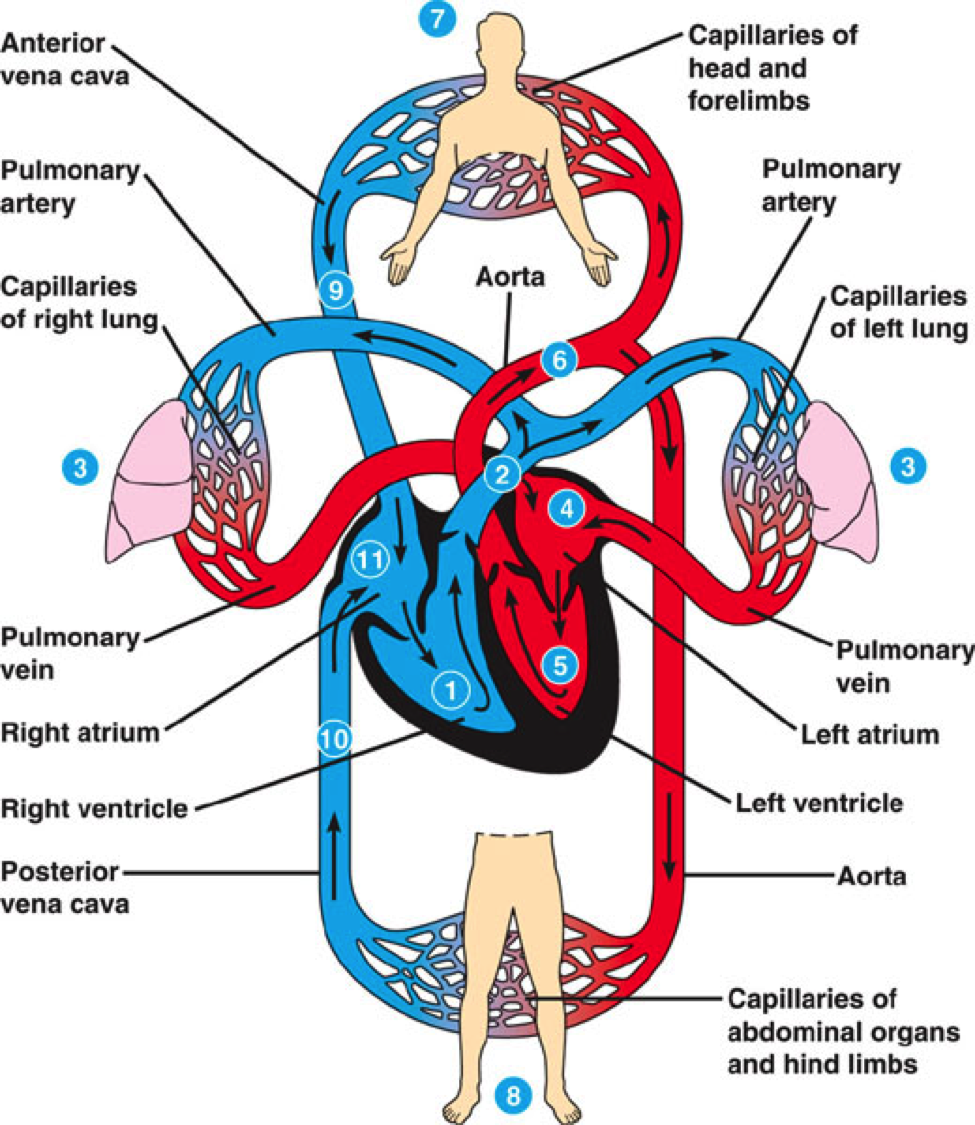

The Cardiovascular system
The cardiovascular (cardio-heart, vascular- blood vessels) system is divided into 2 parts:
- The heart- whose pumping action ensures constant circulation of the blood
- The blood vessels- which forms a lengthy network through which the blood flows.
Blood transports oxygen, nutrients, hormones and other substances to all the cells of the body. It transports waste substances from all the cells of the body. The circulatory system ensures a continuous flow of blood to all the body cells, and its function is subject to continual physiological adjustments to maintain an adequate blood supply.
The blood vessels vary in size, structure and functions, there are several types: arteries, arterioles, capillaries, venules and veins. These blood vessels transport blood away from the heart.
Cardiovascular system

Layers of the heart
The heart is made up of 3 layers of tissue: pericardium, myocardium and endocardium.
- Pericardium- is the outermost layer and is made up of 2 sacs. The outer sac consists of fibrous tissue and the inner of a continuous double layer of serous membrane. There is around 15-50ml of fluid found within the pericardium which reduces friction between the surfaces. The outer fibrous sacs inelastic, fibrous nature prevents overdistenstion of the heart. The serous membrane consists of flattened epithelial cells which secrete serous fluid into the space between the visceral and parietal layers, which allows smooth movement between them when the heart beats.
- Epicardium- is serous membrane of smooth outer surface of the heart. The coronary blood vessels are located here. The Epicardium is part/ can be found within the Pericardium layers.
- Myocardium- is composed of specialised cardiac muscle found only in the heart. It is not under voluntary control but is striated, like skeletal muscle. It forms the atria and ventricles. This muscular layer contains cardiac muscle cells, connective tissues and blood vessels and nerves. This is responsible for the heart contracting.
- Endocardium- This lines the chambers and valves of the heart. it is thin, smooth, glistening membrane that permits smooth flow of blood inside the heart. It consists of flattened epithelial cells, and it is continuous with the endothelium lining the blood vessels.
Layers of the heart

Blood vessels
There are 3 main types of blood vessels:
Arteries- transports blood away from the heart. They vary considerably in size and their walls consist of 3 layers of tissue:
- Tunica adventitia- or outer layer of fibrous tissue
- Tunica media- or middle layer of smooth muscle and elastic tissue
- Tunica intima- or inner layer of squamous epithelium called endothelium.
Arteries have thicker walls than veins to withstand the high pressure of arterial blood.
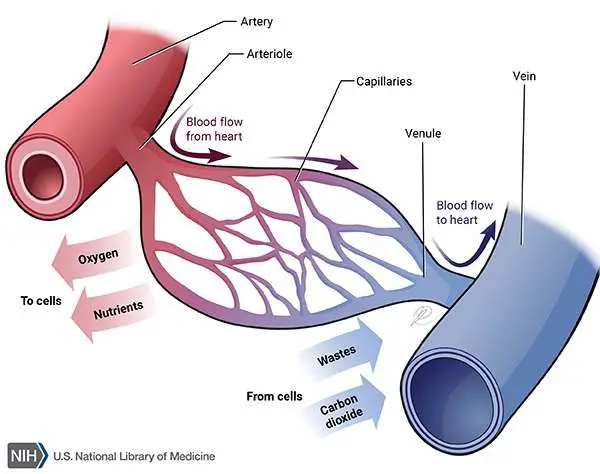
Capillaries/sinusoids- The smallest arterioles break up into a number of minute vessels called capillaries. Capillary walls consist of a single layer of endothelial cells sitting on a very thin basement membrane, though water and other small molecules can pass. Blood cells and large molecules such as plasma proteins do not normally pass through capillary walls. Capillaries form a vast network of tiny vessels that link the smallest arterioles to the smallest veins. They connect arteries and veins.
Veins- are blood vessels that return the blood at low pressure to the heart. The walls of the veins are thinner then those of arteries but have the same 3 layers of tissue. They are thinner because there is less muscle and elastic tissue in the tunica media, because veins carry blood at a lower pressure than arteries.
Each person has about 60,000 miles of blood vessels, about 50,000 miles of those are capillaries.
Blood vessels
The heart

Heart chambers
The atria (left and right atrium)
- Thin walled
- left atrium receives oxygenated blood back from the lungs (via pulmonary veins)
- Right atrium receives deoxygenated blood back from the rest of the body (via the inferior vena cava and superior vena cava)
- Empty into the ventricles below
The ventricles
- Thicker walled than the atria (left ventricle is substantially thinker than the right)
- Left ventricle pumps the blood into the systemic circulation (via the aorta)
- Right ventricle pulps blood into the pulmonary circulation (via the pulmonary artery)
The Heart is a hollow organ that pumps blood deoxygenated blood to the lungs within the pulmonary circuit and oxygenated blood via the systemic circuit. The pulmonary circuit carries deoxygenate blood from the hearts right ventricle (lower right chamber), throught the pulmonary arteries, to the lungs, and oxygenated blood back through the pulmonary veins to the heart's left artium(upper left chamber). The systemic circuit carries oxygenated blood from the left ventricle (lower left chamber), through the systemic arteries and deoxygenated blood through the systemic veins back to the hearts right atrium (upper right chamber).
How the heart pumps blood
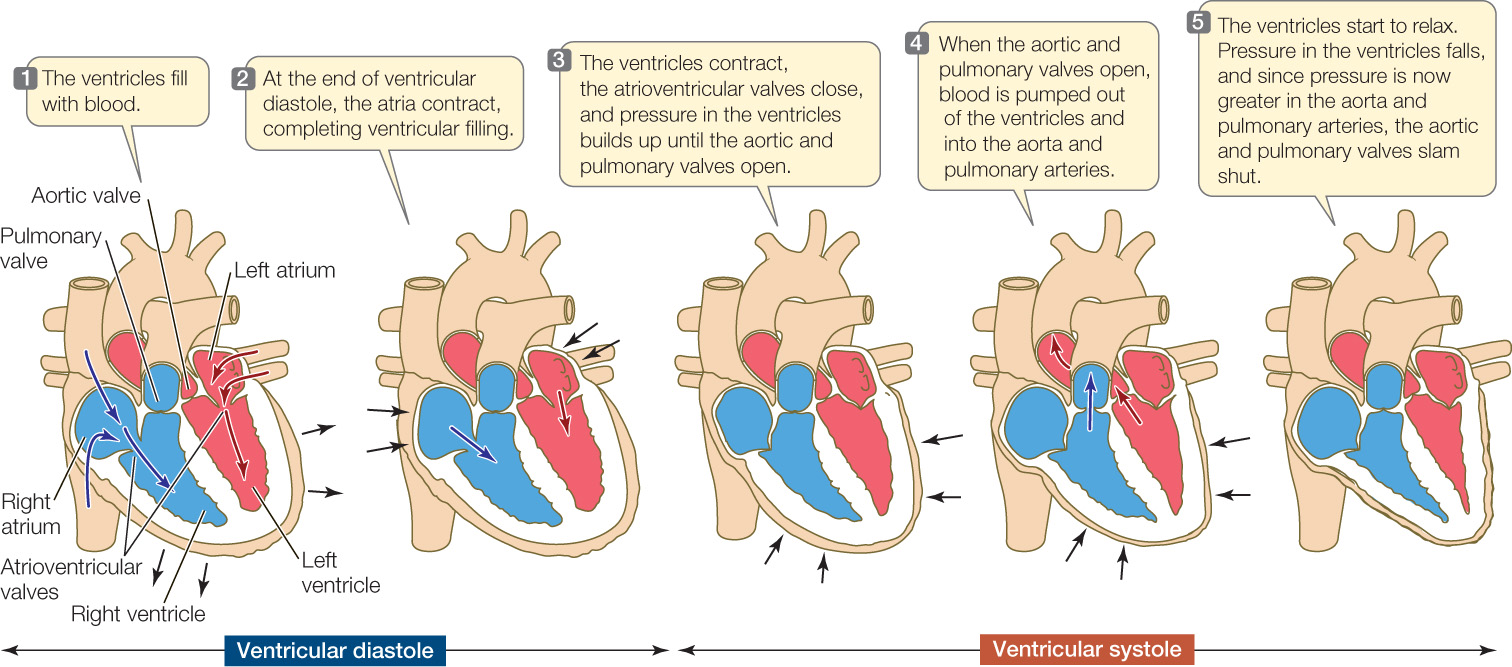
The cardiac cycle
When the cardiac cycle begins, all 4 chambers are relaxed, and the ventricles are partially filled with blood.
1) Both Atria fill at the same time (the heart is resting at this stage known as Diastole)
2) During the Atrial systole the atria contract, filling the ventricles completely with blood (atrial systole lasts 100msec).
3) Ventricle systole begins at the same time as the Atrial diastole. During this period the ventricles push blood through the systemic and pulmonary circuits towards the atria.
The heart then enters ventricular diastole.
For the rest of this cycle, filling occurs passively and both the atria and the ventricles are relaxed. The next cardiac cycle begins with atrial systole, which completes the filling of the ventricles.
Cardiac cycle
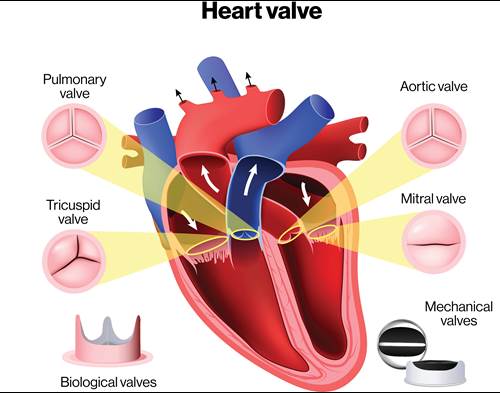
Valves
The valves keep everything moving in a single direction (unidirectional flow) and prevent backflow.
The closing of the valves causes the "lub-dup" heart sound.
Conduction system of the heart
- The heart processes he property of Autorhythmicity, which means it generates its own electrical impulses and beats independently of nervous or hormone control i.e. it is not reliant on external mechanisms to initiate each heartbeat.
- You have a natural pacemaker, the sinoatrial (SA) node which usually dictates how fast your heartbeats due to the fact the SA node discharges faster then any other part of the heart. This small mass of specialised cells lies in the walls of the right atrium near the opening of the superior vena cava.
- The SA node sends electrical impulses through the atria to the Atrioventricular (AV) node and then down the Bundle branches to the Purkinje Fibres in ventricles.
- The Atrioventricular (AV) node is a small mass of neuromuscular tissue when stimulated in the wall of the arterial septum near the atrioventricular valves. Normally the AV node merely transmits the electrical signal from the atria into the ventricles.
SA and AV nodes

Wave of Depolarisation
- 1) SA Node
- 2) Atria
- 3) AV node
- 4) Bundle of His- The bundle of His is an important part of the electrical conduction system of the heart, as it transmits impulses from the atrioventricular node, located at the anterior-inferior end of the interatrial septum, to the ventricles of the heart.
- 5) Bundle branches- The bundle branches, or Tawara branches, are offshoots of the bundle of His in the heart's ventricle. They play an integral role in the electrical conduction system of the heart by transmitting cardiac action potentials from the bundle of His to the Purkinje fibres.
- 6) Purkinje Fibres-The Purkinje fibers( Purkinje tissue or subendocardial branches) are located in the inner ventricular walls of the heart, just beneath the endocardium in a space called the subendocardium. The Purkinje fibers are specialised conducting fibers composed of electrically excitable cells.
- 7) Ventricles
Wave of Depolarisation

P-wave= atria activity, QRE complex= Ventricular activity, T-wave= Everything being "reset"
The Respiratory system
Function of the respiratory system is:
- Providing an extensive surface area for gas exchange between the air and circulating blood.
- Moving air to and from the exchange surfaces of the lungs along the respiratory passageways.
- Protecting respiratory surfaces from dehydration, temperature changes and pathogens.
- Producing sounds for speaking, singing and other forms of communication
- Detecting odors by olfactory receptiors in the superior portions of the nasal cavity
- To allow oxygen to diffuse into blood, so it can be transported to cels throughout the body (to produce energy for things like growth, repair and division)
- To allow carbon dioxide to diffuse from blood to air so that it can be exhaled.
The Respiratory system

Bronchioles
 Roughly 500 milliom alveoli in a set of lungs
Roughly 500 milliom alveoli in a set of lungs
Ventilation
During pulmonary ventilation, we use the respiratory muscles in various combinations, depending on the volume of air that must be moved into or out of the system.
Movement of air from an area of relatively high pressure to an area of relatively low pressure:
Inhalation (active process)
- Diaphragm contracts and flattens, rib cage rises (usually due to contraction of external intercostal muscles)
- Increased chect volume; reduced intrathoracic pressure
- Air is drawn into the lungs
- Elevation of the rib cage and contraction of the diaphragm increases the volume of the thoracic cavity.
- Pressure within the lungs decreases and air flows in
Exhalation (passive process)
- Reversal of process outlined above
- When the rib cage returns to its original position and the diaphragm relaxes, the volume of the thoracic cavity decreases.
- Pressure within the lungs increases and air moves out.
Gas exchange
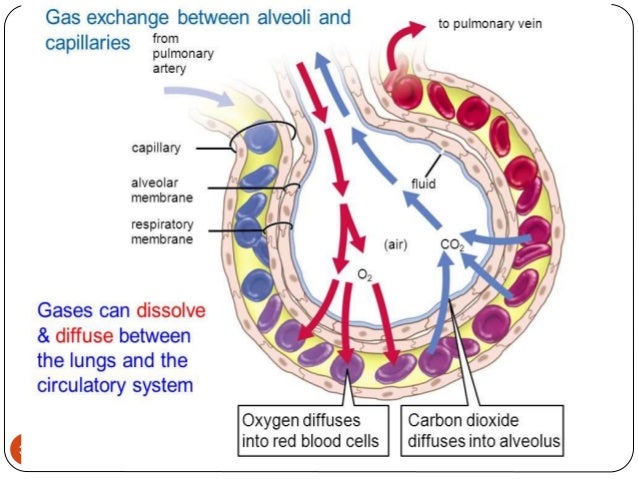
Erythrocytes (red blood cells)
- Contain haemoglobin a complex protein molecule containing iron
- Haemoglobin binds with oxygen forming oxyhaemoglobin
- When haemoglobin binds with the maxium amount of oxygen it can hold it is said to be fully saturated.
- It is possible to measure the level of saturation because of the colour change of the erythrocytes
- Each erythrocyte travels about 12,000 miles a day
Related discussions on The Student Room
- Life as a student nurse at Bradford »
- Pharmacy students at uni »
- pharmacy - struggling with lecture vs textbooks »
- Leeds vs Leicester »
- EPQ suggestions - Pharmacy related »
- NHS Learning Support Fund and Healthcare Science »
- help with dissertation topic »
- Is the respiratory physiologist qualification recognized in countries where...? »
- Cardiac Physiology Applicants 2024 »
- starting child nursing »
Comments
No comments have yet been made