Introduction to ophthalmology
5.0 / 5 based on 1 rating
- Created by: z
- Created on: 13-03-16 13:49
Visual system
- NB: ophthalmology involves whole visual system back to visual cortex
- commonest cause of registered partially sighted and blindness cases for <65 yro is DM
- visual system consists of:
- coordinated pair of eyes
- appropriate protective mechanisms
- neural apparatues to interpret visual info
- eyes:
- form focused image on the retina, dep on:
- ocular shape
- transparency of ocular media
- ability of transparent structures to refract light
- transduction of image into electrical signal
- form focused image on the retina, dep on:
1 of 16
Anatomy of the eye
- retina - light sensitive layer
- cornea - clear window
- iris - colored part
- pupil - hole to lens
2 of 16
Anatomy of the eye: cornea
- cornea:
- transparent
- stroma is relatively dehydrated - maintained by impermiable epithelium (ant.) and active pumping by endothelium (post.)
- b/w regularly spaced stormla collagen fibrils
- refraction
- major refractive component of the eye (not the lens!) - 48/58 dioptre (unit of measurement of optical power of a curved lens)
- barrier to infection and trauma
- layers:
- epithelial cels
- Bowman's membrane
- stroma
- Descemet's membrane
- endothelial cells
- layers:
- NB innerv by CNV1 via short and long ciliary- corneal reflex
- transparent
3 of 16
Anatomy of the eye: sclera
- forms posterior 5/6 of outer coat of eye
- opaque
- mechanically tough
- consists of irregularly arragend collagen fibres
- maintains eye shape
- maintains IOP
- barrier to infection and trauma
- continuous w/ cornea
4 of 16
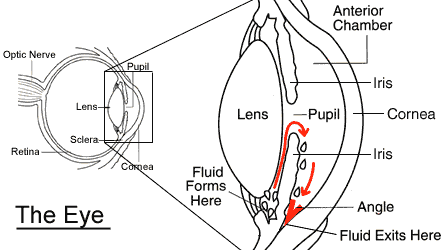
Anatomy of the eye: aqueous humour
- transparent gelatinous fluid, low protein conc
- actively secreted by epithelium of ciliary body
- drained via 2 routes:
- "conventional" (85%) - through trabecular meshwork into canal of Schlemm in anterior chamber angle
- "uvoscleral" (15%) - through ciliary body into ciliary circulation
- balance b/w secretion and drainage determines the IOP
- normal is 10-21 mmHg
- high IOP = glaucoma
5 of 16
Anatomy of the eye: crystalline lens
- transparent:
- orderly arranged lens fibred
- small difference in refractive index b/w various components
- no blood vessels
- fine focusing
- shape changes due to action of ciliary muscles
- close vision: rounder lens as more refraction (accomodation): ciliary muscles contract (parasympathetic) which decr tension in ciliary fibres- allows lens to curve more

- shape changes due to action of ciliary muscles
6 of 16
Ciliary ganglion
- parasymp > ciliary muscles, sphincter pupillae
- symp > dillator pupillae, superior tarsal m. (raises upper eyelid, thus dysfunc=partial ptosis)
- sensory > from cornea (corneal reflex)
7 of 16
Anatomy of the eye: vitreous humour
- transparent, firm gel
- collagen type II, arranged as fibrils
- hyalocytes (only a few) secreting glycosaminoglycan
- protects ocular structures
- is 80% of globe volume
- passive transport and removal of metabolites
8 of 16
Anatomy of the eye: retina
- retina
- transparent
- transduces light energy into nervous impulses
- 11 layers
- photoreceptors - 120 mil rods, 6 mil cones (colour vision)
- macula
- central vision area of the retina, area of highest visual acuity
- lateral to optic disc, visible as slightly darker due to yellow luteal pigment
- fovea lies at centre (cones only)
- optic nerve
- fibres only myelinated after exitting eye
- nasal fibre decussation at optic chiasm
- optic disc
- entry point of nerve into eye
- corresponds to blind spot as no overlying photoRs
9 of 16
Ophthalmic Hx taking
- HPC
- general symtpoms: uni/bilat, onset/duration, any pain/photophobia/redness/discharge etc
- visual symptoms:
- visual loss (sudden/gradual/distortion)
- field defect (uni/bilat. central/peripheral)
- flashes/floaters
- diplopia (horizontal/vertical bino/monocular)
- past ocular Hx (incl refractive Hx e.g. glasses, contacts)
- FHx (esp of ocular disease)
- PMH
- DH/allergies
- general health
- social (ADLs, hobbies able to do?)
- if a child- obstetric/birth details/neonatal complications, milestones, imm Hx
10 of 16
Common ophthalmic symptoms
- "red eye" (pain, redness, photophobia, discharge) > issue at front of eye
- painless loss of vision > back of eye
- distortion of vision/central scotoma > macula
- flashes and floaters > vitreous or retina
11 of 16
Refractive error and accommodation
- emmetropia = no refractive error
- ametropia = error
- myopia: short sighted, light ray scome to focus in front of retine
- either eye is too long (=axial myopia) or lens is to strong (index myopia- due to nuclear sclerotic cataract)
- hypermetropia: long sighted, light ray comes to focus behind the retina
- either the eye is too short or the convergng power of the cornea or lens is too weak
- astigmatism
- cornea is not spherical (instead rugby ball shape)
- myopia: short sighted, light ray scome to focus in front of retine
- accomodation
- allows close objects to be focused on the retina
- ciliayr muscle contracts, suspensory ligaments become lax, naturally elastic lens assumes more globular shape
- with age (>45yrs) lens gradually hardens and becomes unable to accommodate: presbyopia
12 of 16
Ophthalmic examination
- vision
- acuity, fields, colour
- pupils
- light reaction
- front of eye
- pen torch, ophthalmoscope or slit-lamp biomicroscope
- back of eye
- direct or indirect ophthalmoscope
13 of 16
Ophthalmoscopy
- 3 components: lenses, light and diaphragm
- high magnification approx 15x
- small field of view approx 6.5-10 degrees
- thus will not see macula w/ undilated pupil b/c disc will take up whole foeld of view, NB don't get pt to look into light as they will accommodate and make pupil smaller
- lens setting
- keep your glasses on
- remove pt glasses and set according to their refractive error
- ask if they wear glasses
- only for reading? > set to 0
- for distances > long or short sighted?
- if pt doesn't know - look through glasses, if appear smaller they are myopic (red numbers), if larger they are hypermetropic (black numbers). NB if big diff then dial to bigger number
- ask if they wear glasses
14 of 16
Direct ophthalmoscopy
- don't put hand on pts head
- hold ophthalmoscope w/ index finger of lens dial
- angle of approach
- from 15 degrees temproal from pt
- same height as pt
- aim 15 degrees nasal to see optic disc- macula is lateral
- start w/ dominant eye and close the other
- small beam for undilated pupil/lg for dilated (e.g. w/ tropicamide, muscarainic antagonist)
- red reflex
- look at:
- "3 Cs" - cup:disc ratio, colour, contour (margins)
- vessels - arterioles and veins, new/collateral vessels
15 of 16
Diabetic retinopathy
- background retinopaty
- scattered haemorrhages and hard exudates not affecting the macula
- not sight threatening
- diabetic maculopathy
- haemorrhages and hard exudate w/in the macula
- macular oedema
- treated w/ focal laser
- pre-proliferative retinopathy
- > 5 Cotton Wool Spots
- venous changes- thickened, tortuous, beading
- indicates retinal ischaemia
- sight threatening
- proliferative retinopathy
- new vessels to disc (NVD) or elsewhere (NVE) which bleed causing vitreous haemorrhage
- requires extensive laser Rx (panretinal photocoagulation)
16 of 16
Related discussions on The Student Room
- Orthoptics »
- just got the results for my end of third year medical school exam result »
- Optometry to medicine »
- 2024 Medicine Options as an International student »
- my end of third year medical school exam result »
- Oxford Medical Electives »
- Orthoptics »
- Medical Student Electives 2023 »
- Low ucat score »
- Orthoptics Applicants 2023 »
Similar Medicine resources:
0.0 / 5
0.0 / 5
0.0 / 5
0.0 / 5
0.0 / 5
0.0 / 5
3.0 / 5 based on 2 ratings
0.0 / 5
0.0 / 5
0.0 / 5
Comments
Report