Human Reproduction
Male Reproductive system
Female reproductive system
Gametogenesis
Spermatogenesis
oogenesis
sexual intercourse
Fertilisation
Implantation
Sub - fertility
pregnancy testing
- Created by: Ahmra
- Created on: 24-04-13 21:17
Male Reproductive System
- In the Human Reproductive system the gametes are produced in special paired glands called Gonads.
- Male gamete is produced in the testes and the female gametes or egg cells in he ovaries.
- The male system consist of a pair of testes, contained in an external sac, the scrontum; the penis, which is an intromittent organ; genital ducts connecting the two; and various accessory glands which provide constituents for the semen.
- Each testis consists of about a thousand seminiferous tubules which provide the spermatozoa.
- The seminiferous tubules also contain interstitial cells.that produce the male hormone, testosterone.
- When sperm have been produced they collect in the vasa efferentia and then pass to the head of the epididymis where they are mature,
- They then pass along the coiled tube to the base pf the epididymis where they are stored for a short time before passing via the vas deferens to the urethra during ***********.
- Before the vas deferens joins the urethra, it combines with the duct leading from the seminal vesicle to form the ejaculatory duct.
Male Reproductive System Continued.....
The seminal vesicles produce a mucus secretion which helps mobility of the sperm.
- The ejaculatory duct then passes through the prostate gland which produces an alkaline secretion that neutralises the acidity of any urine in the urethra aswell as aiding sperm mobility.
Female Reproductive System
- There are two ovaries each of which produces ova or eggs.
- They are produced in the germinal epithelium where they develop into follicles.
- Mature follicles migrate back to the surface when their development is complete so that the ova can be shed.
- Ova are passed to the fallopian tube ( Oviduct ) which conveys them to the uterus ( womb ).
- The uterus has muscular walls and is lined internally by a mucus membrane called the endometrium.
- It is well supplied with blood and is part of the womb into which the embryo implants during pregnancy and which is shed during menstruation.
- The uterus opens into the vagina through a ring of muscle, the cervix.
Female Reproductive System Continued...
Female reproductive part.
Gametogenesis
The production of gametes in the gonads is known as Gametogenesis.
- Spermatogenesis is the formation of sperm in the testis
- Oogenesis is the formation of eggs or ova in the ovary
The cells of the germinal epithelium of both the testis and the ovary undergo a sequence of mitotic and meiotic divisions to form haploid gametes.
It is important that the gametes are haploid so that at fertilisation the diploid number is restored.
First there is a multiplication stage which involves repeated mitotic divisions to produce spermatogonia and oogonia.
Once formed they grow to full size and then undergo mutation which involves the meiotic division, and then differentiate into the mature gamete.
Spermatogenesis
This is the process by which spermatozoa are produced. This takes place in the germinal epithelium of the seminiferous tubule.
- The diploid spermatogonia divide many times by mitosis to produce primary spermatocytes
- These undergo meiosis and after the first meiotic division haploid secondary spermatocytes
- After the second meiotic division they form spermatids which differentiate int mature spermatozoa
In the wall of the seminiferous tubule are Sertoli Cells. They secrete fluid which nourishes the spermatids ad protects them from the immune system of the male.
There are also groups of interstitial celss which secrete the male sex hormone.
Spermatogenesis Continued...
Oogenesis
- This is the process by which ova are produced in the ovary.
- Oogonia, which are formed before birth, undergo mitosis to form primary oocytes
- Primary oocytes start to divide by meiosis but the process stops at prophase I
- Germinal epithelium also divides to form follicle cells which surround the primary oocytes to form primary follicles. Primary oocytes do not mature until just ovulation.
- About 2 million of these are formed in the ovary of the fetus but only about 450 will develop into secondary oocytes after the onset of puberty.
- At puberty hormones stimulate the follicles to develop further. Each month several follicles start to develop but only one matures into a fully developed Graafian Follicle
- First the primary oocyte completes the 1st meiotic division to form haploid secondary oocyte and a small polar body
- The mature Graafian follicle migrates to the surface of the ovary where it bursts and the secondary oocyte is released, a process called ovulation
- The secondary oocyte begins the secondary meiotic division but this is arrested as Metaphase unless fertilisation takes place.
- On fertilisation this division is completed to form a large ovum & a second polar body.
- Once this division has taken place the nucleus of the ovum fuses with that of the sperm to form a zygote which will then develop into an embryo.
Oogenesis Continued...
Sexual Intercourse
So that fertilisation takes place the sperm has to travel from the seminiferous tubule to the oviduct of the female.
Secretions from the seminal vesicles, Cowper's glands and the prostate gland are added to the sperm to form semen.
The penis of a sexually excited male becomes erect as blood under pressure fills the spongy 'erectile tissue'.
The vagina of a sexually excited female widens and becomes lubricated by the secretion of mucus.
During sexual intercourse the penis is inserted into the vagina. Movement of the penis result in the *********** of semen into the vagina. The force of *********** is sufficient to propel some sperm through the cervix into the uterus, with the remainder being deposited at the top of the vagina.
The sperm swim through the uterus into the oviducts by the lashing movements of their tails. However, only a small proportion, several hundreds of the 400 million sperm actually reach the site of fertilisation in the oviduct and surround the ovum.
Fertilisation
Internal fertilisation ensures that the sperm are deposited in the female's reproductive tract.
From here the sperm use their tails to swim through the cervix and up through the uterus to the oviduct.
The sperm can remain viable for 48 hours. If ovulation has recently taken place there will be a secondary oocyte in the oviduct.
The egg or ovum released from the Graafian follicle of the ovary dies unless fertilised.
The secondary oocyte is surrounded by the follicle cells and a clear membrane called the Zona Pellucida.
Several hundred sperm surround the secondary oocyte but only one will penetrate it.
When a sperm fuses with an egg cell a diploid zygote is formed.
This develops by mitosis to form a mass of cells.
This ball of cells is implanted in the uterus wall where it continues to develop.
The Acrosome Reaction
- Sperm can remain viable for 12 to 24 hous after release into the female tract but can fertilise an ovum only after a process called Capacitation has taken place.
- This process takes several hours.
- It involves changes in the membrane covering the acrosome, a thin cap over the nucleus of the sperm.
- When the sperm reach an oocyte, contact with the zona pellucida results in the acrosome membrane rupturing and protease enzymes are released.
- The emzymes soften the layers of cells surrounding the oocyte.
- Inversion of the acrosome results in a fine needle-like filament developing at the tip of the sperm and this peirces the already softened portion of the membrane.
- The whole process is called The Acrosome Reaction and it enables the sperm to penetrate the egg.
- This entry stimulates reactions of the oocyte that brings about the formation of the fertilisation membrane preventing the entry of further sperm.
- Entry of the sperm also stimulates the completion of the second meiotic division of the oocyte nucleus.
- The nuclei of the ovum and sperm are drawn together and fuse to form diploid nucleus.
Fertilisation Continued....
Implantation
After fertilisation the ovum or zygote begins to divide by mitosis until a hollow ball of cells, the blastocyst, is produced. The development of the zygote continues during its passage down the fallopian tube. After about three days the blastocyst reahes the uterus and embeds in the endometrium. This is called implantation.
Th outer layer of the blastocyst is called trophoblast. This layer develops into two membranes, the amnion and chorion, the latter of which grows a number of finger-like processes called chorionic villi. The villi increase the surface area for the absorption of nutrients from the wall of the uterus. The chorion also secretes a hormone called human Chorionic Gonadotrophin (hCG) which prevents the degeneration of the corpus luteum.
This is the struture which develops from the Graafian follicle after the ovum has been released and is important in hormone production during the early stages of pregnancy. Detection of hCG in the urine is the basis of most pregnancy tests. The chorionic villi eventually form part of the placenta which is attached to the foetus by the umbilical cord.
Sub - Fertility
In the UK, one in six couple,s trying for a baby, seek medical help because of difficulty in becoming pregnant.
Sub - Fertility is defined as difficulty in conceiving naturally for reasons affecting the male, female or both partners.
Infertility is the complete inability to conceive a child; This is very rare.
The greatest cause of female infertility is the failure to ovulate and is usually associated with the absence of, or irregular menstrual cycle.
95% of cases are treatable with the use of a drug called clomiphene.
Another cause of female infertility is a blockage of the fallopian tubes.
This prevents the passage of the ovum to the site of fertilisation in the fallopian tubes.
A blockage may be caused by infection and treatment usually involves microsurgery.
Pregnancy Testing
Most pregnancy testing kits use monoclonal antibodies to test for the presence of hCG in urine. A monoclonal antibody is one that responds to only one foreign antigen. The monoclonal used in the kits is specific to the hormone, hCG.
Pregnancy testing kits involve the detection of hCG produced by the placenta during early stages of pregnancy. The hormone is excreted in the urine and high levels act as a confirmation of pregnancy.
The test relies on the reaction between antibodies bound to coloured latex beads and hCG. It causes the hCG molecules to bind together and produce a colour change.
The kit contains a dipstick, which is a ***** of absorbent material on a plastic backing in which are embedded the antibodies.
The dipstick is placed into a sample of early morning urine and any hCG in the urine will bind to the antibodies at the end of the stick, and will be carried upwards as the urine seeps up the stick.
Pregnancy Testing Continued .....
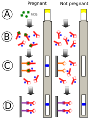 When the hCG - Antibody complex reach the test region in the stick, they bind with the immobilised antibodies there and are held firmly in position.
When the hCG - Antibody complex reach the test region in the stick, they bind with the immobilised antibodies there and are held firmly in position.
As the immobilised antibody complex becomes more and more concentrated there is a colour build-up.
If the test is positive a coloured band becomes visible through a transparent window.
Related discussions on The Student Room
- Advanced Higher Biology Project Ideas »
- bio, biochem, biomed?? »
- AQA Biology essay »
- Career in reproductive/sexual health »
- Where it all started. »
- Who else is vegan on here? »
- Edexcel IGCSE Biology | PAPER 2 »
- Uni Course help »
- Edexcel A Level Biology B Paper 2: 9BI0 02 - 17 Jun 2022 [Exam Chat] »
- Which A-Level Biology should I do? Edexcel A/B »
Comments
No comments have yet been made