11. Communicable Diseases, Disease Prevention and the Immune System
- Created by: zoelaad
- Created on: 30-12-17 16:23
The Different Types of Pathogens
Pathogens are microorganisms that cause disease. The means of transmission can be categorised as direct or indirect. A vector is an organism that carries the pathogen from one host to another.
Pathogens and their means of transmission:
-
Bacteria: tuberculosis (TB)-indirect transmission carried in water droplets, bacterial meningitis-direct contact with saliva, ring rot (potatoes, tomatoes)-direct contact between potatoes
-
Viruses: HIV/AIDS (human)- direct contact with bodily fluids, influenza (animals)-indirect droplet infection, Tobacco Mosaic Virus (plants)-direct contact with spores and indirect vectors
-
Protoctista: malaria-indirect contact via vector, potato/tomato late blight-direct contact with seeds, indirect spores in wind
-
Fungi: black Sigatoka (bananas)-indirect spores in wind, ringworm (cattle)-direct contact with spores, athlete’s foot (humans)-direct contact with spores
Physical Defences used by Plant Against Pathogens
When a pathogen is detected, the following barriers can be enhanced to prevent it spreading through the plant:
- the stomata close to prevent entry to the leaves
- cell walls are thickened with additional cellulose
- callose is deposited between the plant cell wall and cell membrane near the invading pathogen, this strengthens the cell wall and blocks the plasmodesmata
- necrosis (cell 'suicide') - cells surrounding the infection are killed to reduce access to water and nutrients. This is caused by intercellular enzymes that are activated by injury when the cells are killed brown spots are produced on the leaf
- canker- necrosis of woody tissue in the main stem or branch
Chemical Defences used by Plant Against Pathogens
Chemicals such as terpenes and tannins are present to prevent the entry of pathogen. However, if pathogens do enter the plant, other chemical defences include:
- terpenoids- essential oils with antibacterial and antifungal properties
- phenols- found in bark, which has antibiotic and antifungal properties
- alkaloids- give a bitter taste to inhibit herbivorous feeding. they also interfere with metabolism by inhibiting or activating enzyme reactions
- defensins- small cysteine-rich proteins that inhibit ion transport channels in plasma membranes of pathogen cells
- hydrolytic enzymes- found in the spaces between cells, these break down the chitin in fungal cell walls which hydrolyse the glycosidic bonds in bacterial walls
Animal Defences Against Pathogens 1
Primary Defences- prevents the entry of the pathogens into the body
Secondary Defences- combats pathogens that have already entered the body
Primary Defences:
- Blood Clotting and Skin Repair- Blood clots reduce the loss of blood and make a temporary seal, preventing access to pathogens. Blood-clotting involves calcium ions and at least 12 other clotting factors that are released by platelets or the damaged tissue. These factors activate an enzyme cascade, which produces insoluble fibres. The clot dries out to form a scab. The scab shrinks over time and forms new skin.
- Inflammation- This is the swelling and redness seen in infected tissues. This is caused by cell-signalling substances called histamines. Histamines cause vasodilation and makes the capillary walls more permeable to white blood cells and some proteins. More plasma enters the tissue fluid which causes the swelling. The excess tissue fluid is drained into the lymphatic system, moving the infecting pathogens toward the lymph nodes where the lymphocytes can start the specific immune response
- Mucous Membranes- Any areas where the skin is incomplete are protected by mucous membranes. The mucus produced by goblet cells trap any pathogens, immobilising them. Some areas have cilia to waft the mucus away (e.g in the airways). Mucous membranes are sensitive to irritation. This causes expulsive reflexes (coughing, sneezing and vomiting). This is a response to the presence of microorganisms and toxins.
Animal Defences Against Pathogens 2
Secondary Defences:
The Non-Specific Immune Response
- Phagocytosis- This involves phagocytic white blood cells (neutrophils) that engulf and destroy any non-self cells. Non-self cells are recognised because they have antigens that do not match the host's antigens. They may also be identified by non-specific antibodies that bind to the pathogen. Phagocytosis follows a particular sequence:
- the bacteria are engulfed by the neutrophil
- they are surrounded by a vacuole called a phagosome
- lysosomes fuse to the phagosome
- lytic enzymes are released into the phagosome
- the bacteria are digested and the nutrients can be reabsorbed by the cell
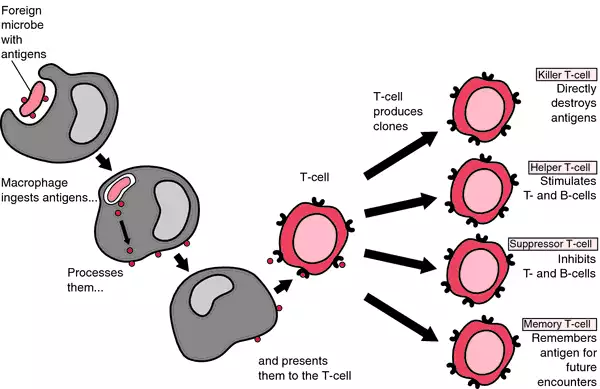
- Antigen Presentation- Macrophages can engulf the pathogen and process it so that the antigen is kept whole. This antigen can then be placed in a special protein complex on the cell surface membrane. This is known as antigen presentation. These antigen-presenting cells can then be used to initiate the specific immune response.
Animal Defences Against Pathogens 3
The Specific Immune Response
1. Antigen Presentation
2. Clonal Selection: There may only be a few lymphocytes that have the correct receptors to bind to the antigens. B lymphocytes, T Helper lymphocytes and T Killer lymphocytes cells must be found and activated to respond. They are selected and activated by coming into contact with the specific foreign antigen. This ends the cell-signalling role of the antigens presenting cell. The action of macrophages makes this selection more likely.
3. Clonal Expansion and Differentiation: Once activated, the specific lymphocytes increase in numbers by mitosis. Cells from the clone of B lymphocytes will differentiate into plasma cells and Memory cells. The plasma cells are short-lived. They produce and release the antibodies which are proteins that have specific binding sites and are capable of acting against the pathogen
4. Differentiation: Cells from the T Helper lymphocytes clone will differentiate into T Helper cells and Memory cells. The T Helper cells secrete hormone-like substances called cytokines and interleukins that help stimulate the B lymphocytes and the macrophages. Memory cells are long-lived and remain in the blood, providing immunological memory and long-term immunity. If the same pathogen invades again, it will be recognised and attacked more quickly. The T Killer clones manufacture harmful substances and attack and kill host cells that are infected. T Regulator cells have a role in closing down the immune response once the pathogen has been removed.
Animal Defences Against Pathogens 4
Primary and Secondary Immune Responses
Primary Responses:
The first time a pathogen invades the body, it produces a primary response. This takes a few days as the specific B and T lymphocytes must be selected, the cells must divide and then differentiate and the antibodies must be manufactured. As a result, the peak of activity and the maximum concentration of antibodies are not achieved until several days after infection.
Secondary Responses:
On any subsequent invasion by the same pathogen with identical antigens on its surface, the immune response is a secondary response. The immune system can respond much more quickly and with higher intensity. This is because of the blood carriers many memory cells that are specific to this pathogen. They divide and differentiate into plasma cells, which manufacture antibodies. The response is quick enough to prevent the pathogen taking hold and causing symptoms of illness.
The Structure and Function of Antibodies
The General Structure:
Antibodies are large globular proteins. Most antibodies are similar in structure and posses the same basic components. They consist of four polypeptides held together by disulfide bridges
- One end of an antibody is known as the constant region, this has a binding site that can be recognised by phagocytes
- The opposite end is known as the variable region, this has binding sites that are specific to particular antigens. They have a shape that is complementary to the shape of the antigen.
- The antibody molecule also has a hinge region that allows some flexibility to enhance binding to more than one pathogen
The Action of Antibodies:
- Opsonins- Antibodies that bind to a pathogen and help phagocytes to bind
- Agglutins- Antibodies that bind to two or more pathogens so that they are held together. This prevents them entering cells and reproducing.
- Anti-toxins- Antibodies that bind to the toxin, making it harmless

Types of Immunity
Active and Passive Immunity:
Active Immunity- Acquired through activation of the immune system. It involves the selection of specific lymphocytes and the production of antibodies and memory cells
Passive Immunity- Acquired from another source. Antibodies may be injected straight into the blood or acquired from a mother's milk. These antibodies do not last long, but they do give immunity from a specific pathogen. No memory cells are made, so the immunity is not permanent
Natural and Artificial Immunity:
Natural Immunity- Acquired in the course of everyday activity. Maybe the result of catching a flu virus from someones sneeze. Natural passive immunity may be acquired through breastmilk or the placenta
Artificial Immunity- Acquired by human intervention. Maybe the result of a vaccination. Artifical passive immunity results from an injection of antibodies
The Principles of Vaccination
Routine Vaccinations
Vaccinations are the deliberate introduction of antigenic material in order to stimulate the production of antibodies. The antigenic material can be:
- whole live microorganisms (more effective than using dead ones as the live organisms can reproduce and mimic an infection better)
- dead microorganisms
- weakened organisms
- a surface preparation of antigens
- a toxoid (a harmless form of toxins)
Herd and Ring Vaccination
In order to be effective, vaccinations need to be used appropriately. Herd vaccination involves the systematic vaccination of all or most members of a population. This prevents the pathogen being transmitted from person to person. Ring vaccination is a response to an outbreak. All the people in the area surrounding the outbreak are vaccinated in order to prevent transmission and to isolate the outbreak in one area
Possible Sources of Medicines
New Medicines:
Microorganisms and plants produce a wide range of molecules that may be of benefit in fighting disease. In the natural world, there may be organisms that produce chemicals that are beneficial against a wide range of pathogens and diseases. Every species that becomes extinct could potentially hold the cure for a major disease. Therefore it is important to maintain diversity.
Personalised Medicine-
Screening the genomes of many plants and microorganisms enables scientists to identify compounds that may have a medicinal value. As technology techniques improve, it may be possible to sequence the DNA of an individual to assess a specific genetic disorder and develop treatment personalised to the individual, such as an individual combination of drugs.
Synthetic Biology-
Scientists can modify natural molecules for use as medicines. Synthetic biology is the development of new molecules or systmes. This could be making new enzymes to create a new product or using natural enzymes to produce a new effect. For example, bacteria are being genetically modified for use as biosensors. Scientists created new pathways that enable bioluminescent bacteria to release light in response to specific pollutants.
Benefits and Risks of Antibiotics
- The first antibiotic, penicillin, was discovered by Alexander Fleming in 1928
- Since then, many different antibiotics have been discovered and used widely to treat bacterial infections
- The use of antibiotics became widespread during WW2 to prevent the infection of wounds
- However, their misuses has enabled microorganisms to develop resistance
- Clostridium difficile (C. diff) and methicillin-resistant Staphylococcus aureus (MRSA) are well known for their multiple resistance to antibiotic
Related discussions on The Student Room
- Why am I prone to infection »
- Plano primary care »
- OCR A-Level Geography Geographical Debates | [12th June 2023] Exam Chat »
- Please give advice which course to choose? (UCL, Queen Mary) »
- EPQ suggestions - Pharmacy related »
- OCR Biology »
- Research Project Question »
- Vaccinations for Thailand »
- Disadvantages of chemical barriers »
- World Cancer Day - Careers »
Comments
No comments have yet been made