Blood and Circulation
- Created by: Jacqui2
- Created on: 27-04-17 09:52
Double Circulatory System
Low pressure in the pulmonary circulation pushes blood slowly into the lungs allowing more time for gas exchange. The high pressure in the systemic circulation ensures blood is pumped to all the other body organs.
Veins and Arteries

Arteries
- More elastic tissue - blood is under high pressure - Tunica Media allows walls to stretch and recoil
- Small lumen - high pressure
Veins
- Have a large lumen - blood is at low pressures
- Semi-lunar valves - prevent backflow
Atherosclerosis and Atheroma
Atherosclerosis - artery wall thickenss as a result of a build up of fatty materials
1). Endothelium lining the artery becomes damaged. Can result from high blood pressure which puts extra strain on the cells.
2). Causes an inflammatory respons. Macrophages leave the blood vessel and into the artery wall. These accumulate from chemials in the blood, particulary cholesterol. A deposit builds up which is called an atheroma.
3). Hard swelling, phagocytes are released, and cause a build up of plaque on the inner wall. Build of up fibrous tissue means the artery wall loses its elasticity
4). Plaque causes the artery wall to narrow which makes it difficult for the artery to stretch and reocil. This makes it difficult for the heart to pump blood around and therofre blood pressure is increased
Coronary Thrombosis
- If a fatty plaque breaks off an artery, cholestrol is released which leads to a rapid clot formation
- A clot that forms inside a damaged but intact blood vessel is called a thrombus
- The condition is thrombosis
- If it happens inside a cornary artery it is called a cornary thrombosis and this starves the heart muscle of oxygen.
- It may lead to mycocardial infarction or, if a large artery is blocked, cardiac arrest
Capillaries
- One cell thick composed of squamous endothelium with gaps between cells
- Tissue fluid is forced out through the high hydrostatic pressure of the blood coming from the heart
- It is drawn back into the capillary by osmosis as its contents remain concentrated

Aneurysm - repture in blood vessel causing blood to escape whch can result in a stroke
Structure of the Heart
Functioning of the Heart
Cardiac muscle is myogenic, it can create and sustain its own contraction without the need for nervous or hormonal stimulation
- Contraction of the heart is known as systole and relaxation as diastole
- Atrio-ventricualr valves are made from connective tissue and ensure one way flow
- Right hand side - tricuspid valve. Left hand side - bicuspid valve
- The chordae tendinae prevent the av vales blowing inside out so prevent backflow into the atria
- Semi-lunar valves also prevent backflow of blood into the ventricles and are made from connective tissue however do not have chordae tendinae
Cardiac Cycle
During this time, the two sides of the heart are synchronised. The left hand side pumps blood to the body while the right hand side pumps blood to the lungs. Therefore the left wall is thicker to allow a greater force of contraction to generate greater pressure to pump the blood further.
1). Atrial Systole
- The contraction of the atria causes the pressure of blood in the chamber to increase.
- This causes the atrioventricular valves to be forced open allowing teh remainder of the blood into the ventricles
2). Ventricular Systole
- The muscular walls of the ventricles contract and the pressure rises
- When the pressure of the blood in the ventricles increase that of the artia the atrioventricular valves shut
- The pressure of the ventricles will also exceed that of the arteries leaving the heart and this will force open the semilunar valves allowing blood to leave the heart
3). Diastole
- Ventricles relax and pressure decreases to that of the arteries causing the semilunar valves to shut
- Blood will enter the artia via veins
Graph of Cardiac Cycle
Nerve Conduction Pathway
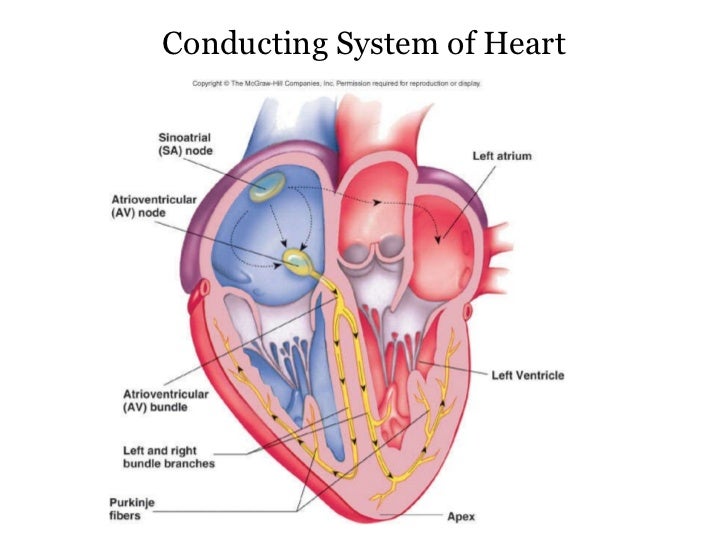
Waves of Excitation
The Sinoatrial Node (SAN) is located in the wall of the right atrium. The are acts as a pacemaker for the rest of the heart. The cells are myogenic. Excitation from the SAN spreads out smoothly across the atria, producing atrial systole. The contraction is prevented from spreading directly to the ventricles by the thin layer of connective tissue along the AV valves. Consequently, excitation must pass to the ventricles by the way of the Atrioventricular Node (AVN), located near the base of the atria.
There is a slight delay (about 0.1s) in order to allow time for the ventricles to completey fill with blood before ventricular systole. From the AVN, connecting fibres in the bundle of his rapidly carry the excitation wave down through the walls of the ventricles and back up throuh the perkinje fibres. Thus ventricualr systole begins at the bottom of the heart and spreads upwards, squeezing blood up out from the ventricles into the arota and pulmonary artery.
Electrocardiogram
P - spread of electrical activity over the surface of the artia leading to..
QRS Complex - spread of electrical activity over the ventricles leading to..
T Wave - electrical recovery of the ventricles and atrai allowing the two to relax and fill with blood
Body Fluids
- Plasma -
- Transports products of digestion, ions, carbon dioxide, urea, heat, prothrombin, fibrinogen and clotting factors
- Monocytes/Macrophages -
- Phagocytic, ingesting bacteria and other large particles. A mature monocyte
- Lymphocytes -
- Respond to foreign substances, antigens.
- T-cells direcctly attack and destroy foreign cells.
- B-cells make antibodies;- antibodies attach to antigens on foreign cells inactivating, clumping or destroying them
- Polymorphs/Microphages -
- Lobed nucleus and grainy cytoplasm.
- Phagocytic engulfing and digestiong disease cauing bacteria
- Digested inside vesciles by lysozymes
- Red cells/Erythrocytes -
- Transport oxygen
- Small size allows oxygen to be picked up and readily released
- No nucleus or mitochondria - allows more haemoglobin
- Biconcave discs. Large surface area and a large volume
- Transport oxygen
Body Fluids
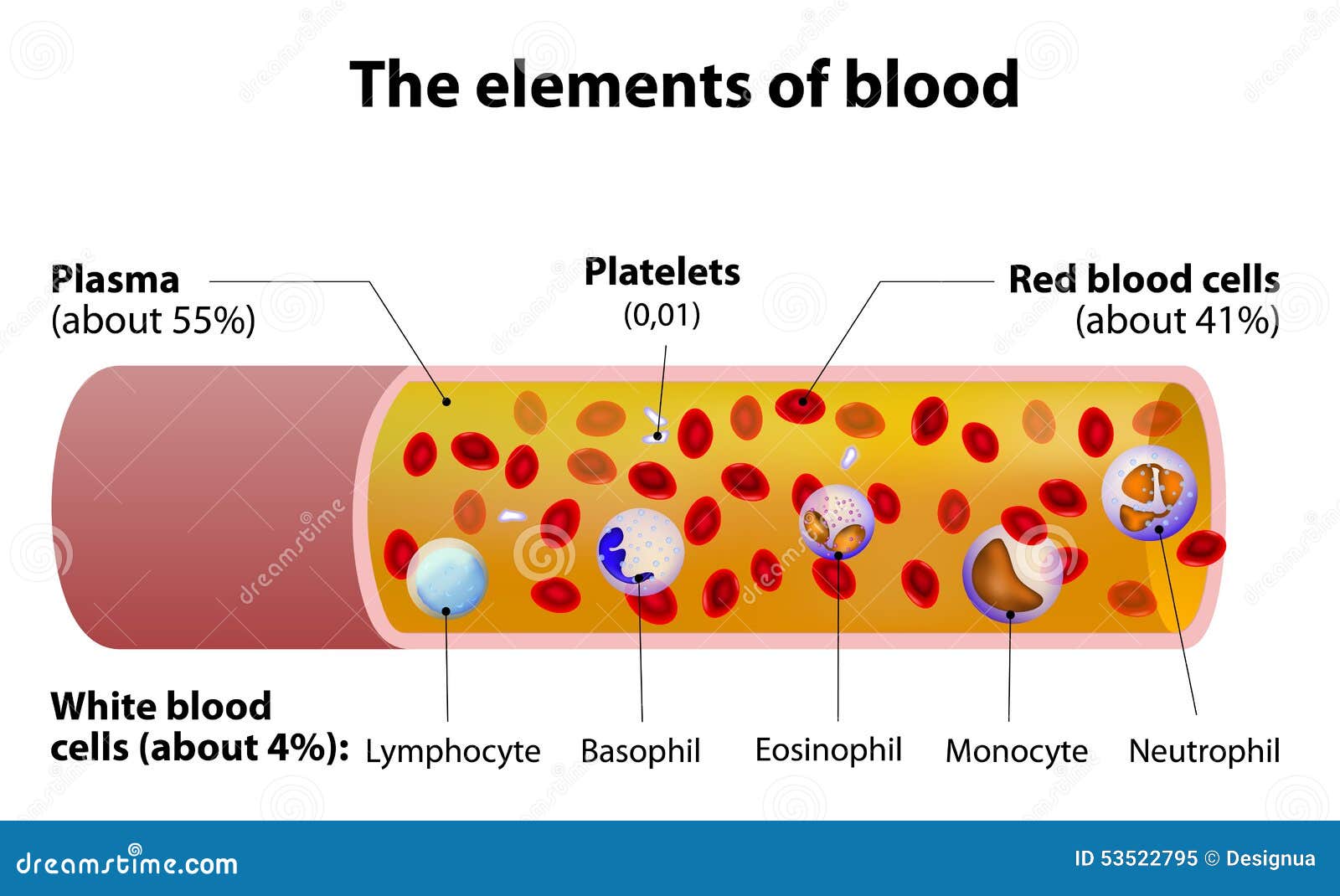
Basophil, Eosinophil and Neutrophil - Polymorphs
Blood Clotting

- Platelets initiate the mechanism of blood clotting
- Thromboplastin is released by platelets to set off a sequence of events
- Conversion of Prothrombin to Thrombin (presence of calcium and vit K)
- Conversion of Fibrinogen to Fibrin by thrombin which form clot
If a clotting factor is not present (calcium, vit K), blood will not clot
Haemoglobin
- Is a conjugated protein - prosthetic group haem
- Consists of 4 polypeptide chains
- Each haem consists of iron and each haem group can combine with one molecule of oxygen
- The binding of the first oxygen enhances the binding to the second haem
- Ensures rapid saturation - sigmodial curve
- At high pp (lungs) haemoglobin is well saturated with oxygen
- At low pp (muscles) haemoglobin has a lower saturation of oxygen as it unloads it
- Ensures rapid saturation - sigmodial curve
Effect of Altitude on Oxygen Transport by Heamoglo
- Partial pressure of oxygen in teh air is low at high altitudes
- Those who live/train at high altitudes have greater numbers of red blood cells which allows for more efficient delivery of oxygen.
- Heamoglobin tends to saturate more readily with oxygen
- More mitochondria
- Increased myoglobin
Bohr Effect
With an increase in carbon dioxide and temperature the curve moves to the right, which allows haemoglobin to release more oxygen.
This results in an increased oxygen supply to tissues where the demand for oxygen has increased due to increased respiration. As there is more carbon dioxide being produced, haemoglobin is more willing to give up its oxygen
Myoglobin
- Oxygen transporting pigment found in red muscle
- The dissociation curve for myoglobin is dispalced to the left to that of haemoglobin
- Myoglobin has a higher affinity for oxygen, causing myoglobin to remain saturated at lower partial pressures
- This is an adaptation to ensure muscle metabolism can remain aerobic at lower pp of oxygen. This delays the onset of anaerobic respiration
- Anaerobic respiration also builds up the toxic waste product lactic acid
- Hence, myoglobin acts as a reservoir of oxygen. It only gives it away when pp are very low.
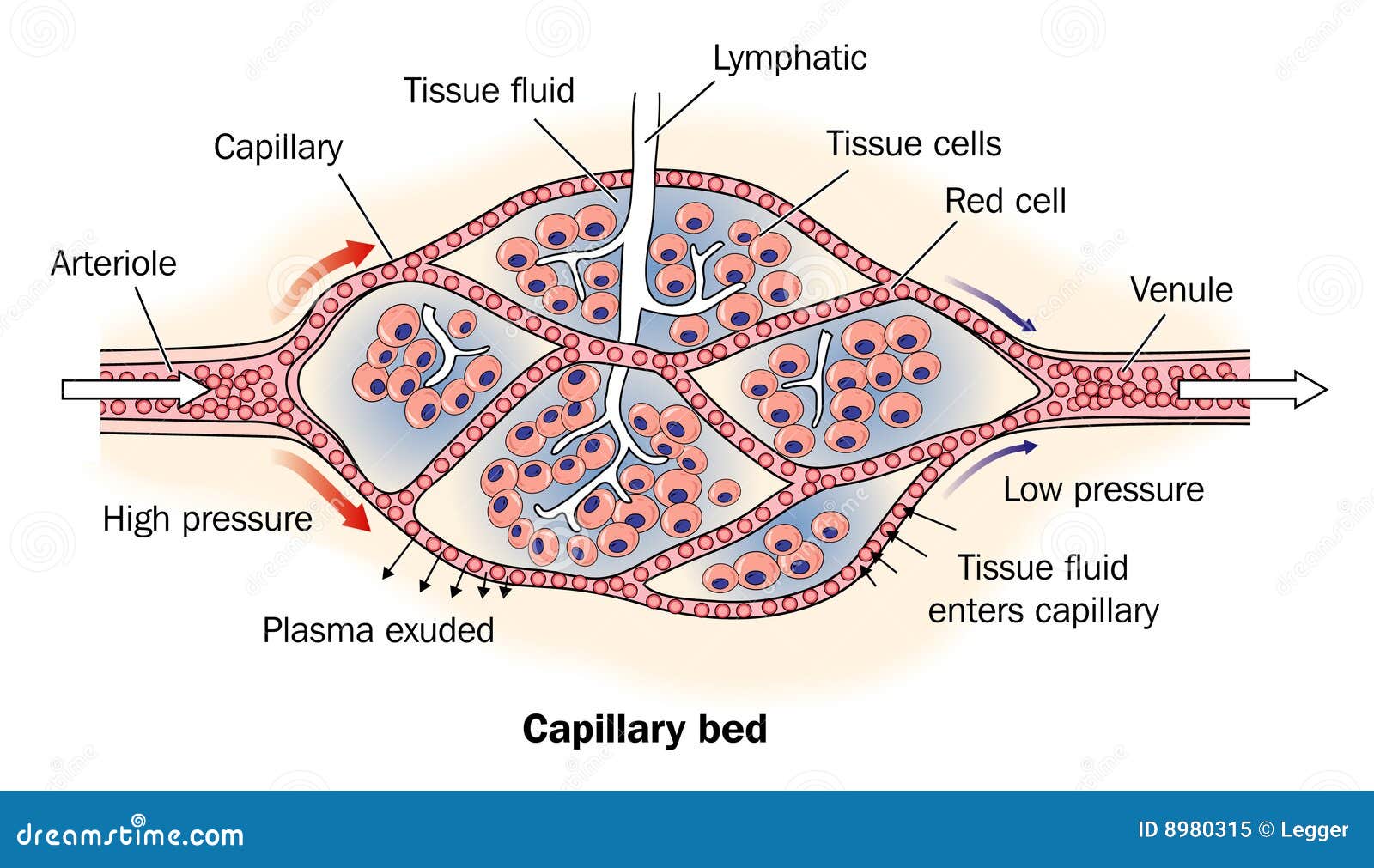
Tissue Fluid Formation and Reabsorption
- Liquid that leaves capillaries to supply cells with nutrients (glucose, amino acids, vitamins etc) and oxygen and helps remove waste products such as CO2 and urea
- It is formed at the arteriole end of vcapillaries and returns back to the blood stream by osmosis at the venule end.
Two factors govern whether or not tissue fluid enters or leaves capillaries. These are:
- HYDROSTSTIC PRESSURE - due to the pressure of the blood genertaed by the contraction of the heart
- OSMOTIC PRESSURE - due to teh presence of solutes in the plasma. These make the plasma a concentrated solution wich will tend to draw water/tissue fluid into the capillary.
Related discussions on The Student Room
- Predictions for Blood Brothers AQA English Lit question on Friday 25th »
- Why i have this vein?! »
- This Classic School Problem Nobody Talks About! »
- Retinol »
- Economics study help »
- Reynaud's »
- Help with a reference to a historical source from Scotland »
- University spreadsheets »
- Atmospheric circulation »
- Your best ways to beat the heat and stay cool? »
Comments
No comments have yet been made